Managing Inflammatory Bowel Disease (IBD): A Comprehensive Guide to Ulcerative Colitis and Crohn’s Disease Treatment

Inflammatory bowel disease (IBD) is a chronic condition that affects millions of people worldwide. There are two main types of IBD: ulcerative colitis and Crohn’s disease. Both conditions cause inflammation in the digestive tract, which can lead to symptoms such as abdominal pain, diarrhea, and rectal bleeding. While there is currently no cure for IBD, there are many treatment options available to help manage the symptoms and improve quality of life.
As many as 780,000 people in the United States are affected by Crohn’s disease, making it a widespread ailment. The disease is most prevalent in people between the ages of 15 and 35, with 25% of cases being identified by age 20. Crohn’s disease is a kind of inflammatory bowel disease (IBD).
In this comprehensive guide, we will explore the different treatment options available for managing ulcerative colitis and Crohn’s disease, as well as lifestyle changes and self-care practices that can help alleviate symptoms and improve overall health.
Understanding Ulcerative Colitis and Crohn’s Disease
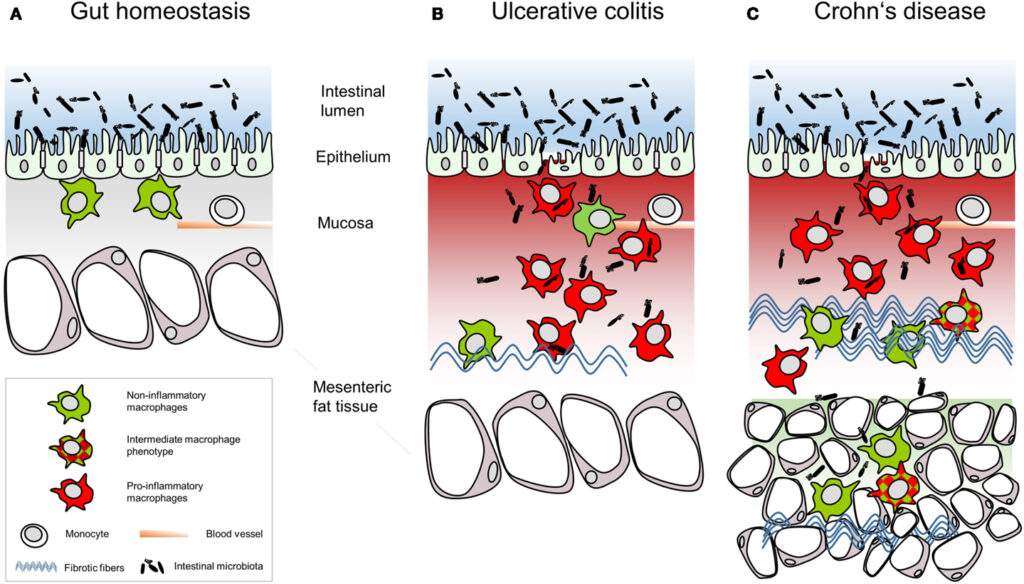
Ulcerative colitis and Crohn’s disease are both inflammatory bowel diseases that cause chronic inflammation in the digestive tract. Ulcerative colitis affects only the colon (large intestine) and rectum, while Crohn’s disease can affect any part of the digestive tract, from the mouth to the anus.
Symptoms of ulcerative colitis may include:
- Diarrhea
- Abdominal pain and cramping
- Rectal bleeding
- Urgency to have a bowel movement
- Weight loss
Symptoms of Crohn’s disease may include:
- Abdominal pain and cramping
- Diarrhea
- Rectal bleeding
- Fatigue
- Fever
While the exact causes of IBD are not known, it is believed to be a combination of genetic and environmental factors. Stress, certain foods, and other triggers can also exacerbate symptoms.
Treatment Options for Ulcerative Colitis and Crohn’s Disease
There are several different treatment options available for managing the symptoms of ulcerative colitis and Crohn’s disease. The most common treatments include medication, lifestyle changes, and surgery.
Medication
Medication is often the first line of treatment for IBD. The type of medication prescribed will depend on the severity and location of the inflammation, as well as other factors such as the patient’s age and overall health.
Some common medications used to treat IBD include:
- Anti-inflammatory drugs: These medications help reduce inflammation in the digestive tract, and may include corticosteroids, aminosalicylates, and immunomodulators.
- Biologic therapies: These medications target specific proteins in the immune system that contribute to inflammation. Biologics are often used in more severe cases of IBD.
- Antibiotics: Antibiotics may be used to treat infections that can exacerbate symptoms of IBD.
- Pain relievers: Over-the-counter pain relievers such as acetaminophen may be used to alleviate mild pain, but nonsteroidal anti-inflammatory drugs (NSAIDs) should be avoided as they can worsen symptoms.
Lifestyle Changes
In addition to medication, lifestyle changes can also help manage the symptoms of IBD. Some lifestyle changes that may be helpful include:
- Diet: While there is no specific “IBD diet,” some people find that certain foods can exacerbate symptoms. Keeping a food diary and working with a registered dietitian can help identify trigger foods and create a personalized nutrition plan.
- Stress management: Stress can exacerbate symptoms of IBD. Relaxation techniques such as meditation, deep breathing, and yoga can help reduce stress and improve overall well-being.
- Exercise: Regular exercise can help reduce inflammation and improve overall health. Low-impact exercises such as walking, cycling, and swimming are often recommended for people with IBD.
- Quit smoking: Smoking can exacerbate symptoms of IBD, and quitting smoking can help improve symptoms and reduce the risk of complications.
Surgery
In some cases, surgery may be necessary to manage the symptoms of IBD. Surgery may be recommended if medication and lifestyle changes are not effective in managing symptoms, or if there are complications such as intestinal blockages or perforations.
There are several different types of surgery that may be performed for IBD, including:
- Colectomy: This surgery involves removing the entire colon. It may be necessary in severe cases of ulcerative colitis that do not respond to other treatments.
- Proctocolectomy: This surgery involves removing both the colon and rectum. It is often used to treat severe cases of ulcerative colitis.
- Strictureplasty: This surgery is used to treat strictures (narrowing) in the intestines caused by Crohn’s disease. The narrowed area is widened by making a longitudinal incision in the intestine and suturing it transversely.
- Ileostomy: This surgery involves creating a permanent or temporary opening (stoma) in the abdomen for waste to pass through. It may be necessary if the rectum is removed.
Self-Care Practices for Managing IBD
In addition to medical treatments and lifestyle changes, there are several self-care practices that can help manage the symptoms of IBD:
- Keep a symptom diary: Keeping track of symptoms can help identify triggers and track progress.
- Stay hydrated: Drinking plenty of water can help prevent dehydration caused by diarrhea.
- Get enough rest: Fatigue is a common symptom of IBD, and getting enough rest is important for overall well-being.
- Join a support group: Joining a support group can help connect with others who understand what it’s like to live with IBD and provide emotional support.
Conclusion
Inflammatory bowel disease can be a challenging condition to manage, but there are many treatment options available to help alleviate symptoms and improve quality of life. Medication, lifestyle changes, surgery, and self-care practices can all play a role in managing IBD. It’s important to work closely with a healthcare provider to develop a personalized treatment plan that meets individual needs and preferences. With the right treatment and self-care practices, many people with IBD are able to live full, active lives.